Survey among medical professionals
To develop tools that are best adapted to the needs of health professionals, SEX-ED + circulated a survey in November 2020, asking doctors, nurses, OB/GYNs, midwives, physios, sexologists or any other medical professional, to complete it.
Questions were about the sexual health received during med school (if at all), the topics covered and the pedagogical tools used during class and training. The goal is to understand better what health professionals have been taught while in school, which pedagogical supports they had access to and if they felt ready to support their patients in their sexual health journey at the end of their training.
*** Consult the survey here ***
The results were shared on social media and are now agregated on this page. CLick on the pictures to get the slides moving.
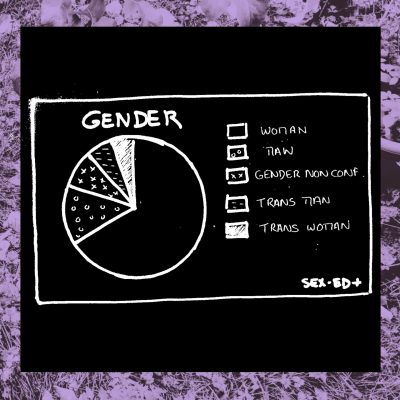
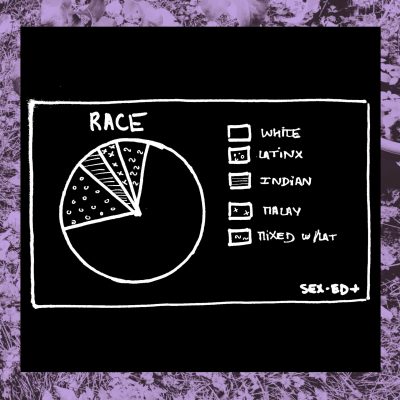
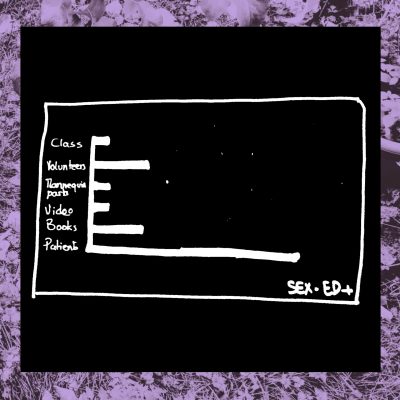
1- Who answered the survey?
2- How many hours of sexuality education training do medical professionals receive during their school years?
In 2014, the article “The state of sexual health education in US medicine” showed that only 55% of medical schools had a sexual health curriculum. Schools reported that they provided a median of eight hours of clinical education on sexual health topics. Yup. Half of future MDs do not have sexual health training. The other half has got a day training. Over their whole medical school years.
To say that there is a chance that they are not adequately trained on sexual health matters may be an understatement. Yet, those people are at the front line as they are the ones we are most in contact with during our health journey.
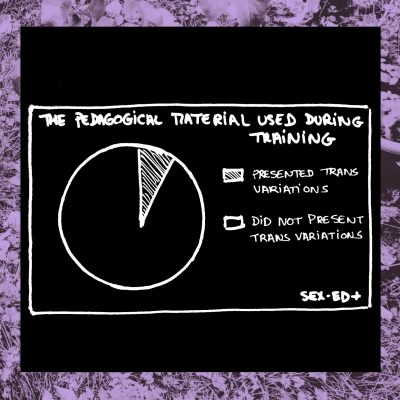
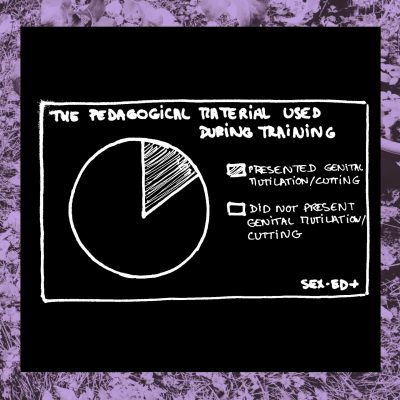
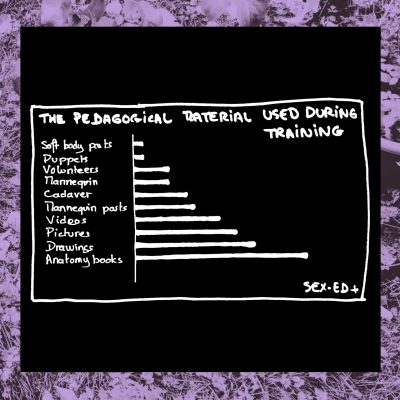
3- What are the topics covered during med school?
Why are we so bent on providing adequate tools for the training of medical professionals? Because they need it to be trained adequately, in a way that is respectful of themselves and others. Be aware that one slide contains elements of gynecological violence.
One’s mission as a health professional is to give the best quality of care to one’s patients, whatever their bodies, identities or experiences.
But is it really possible when one is only taught about certain types of bodies? It is as necessary to know cisgender bodies than it is to know trans bodies, Intersex bodies and cut/mutilated bodies. Because they exist and deserve care, respect and knowledgeable medical professionals.That is why we advocate for pedagogical tools that represent the diversity of bodies and genitals.
Better trained health professionals= better care for patients.
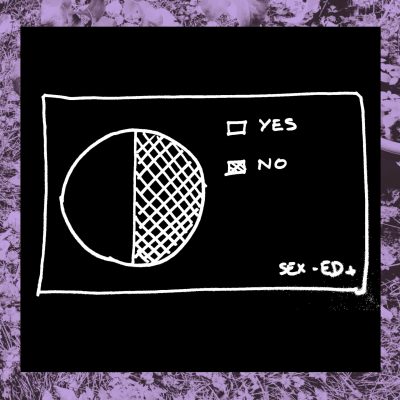
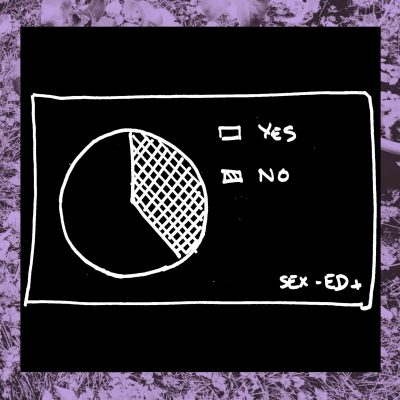
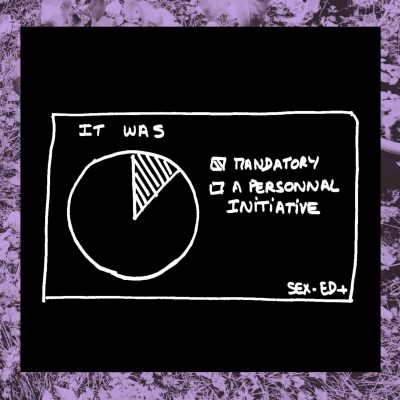
4- Is it required for health professionals to keep up to date with sexual health knowledge?
Not only is there very little sexuality and sexual health education during medical training, but there is also little mandatory training to keep up to date with the subject once out of school. It may explain why a gynecologist once refused to give me an IUD because I had never been pregnant before…NOTE: you can totally use an Intra Uterine Device for contraception even if you have never been pregnant. It is actually a very effective and safe method
Most of the folks who answered our survey actually took it upon themselves to improve their knowledge by volunteering, taking extra classes, reading, attending conferences (thank you for that ). But those are the ones who think that sexual health is an important part of their job and who know that their training was not complete.
What about those who don’t know that they don’t know ? I guess they are still out there, giving 40 years out of date information about contraceptive methods 🙁
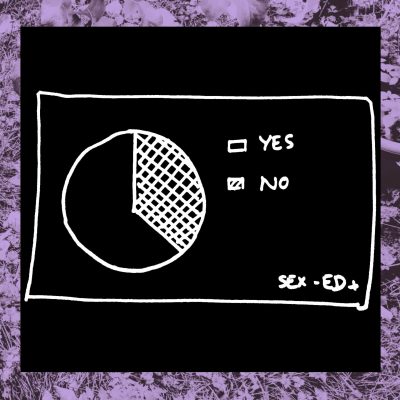
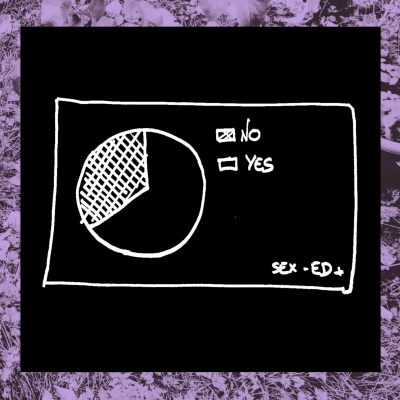
5- Are medical professional prepared to talk about sexual health?
Further reading:
- “Sexual Health Competencies for Undergraduate Medical Education in North America” Carey Roth Bayer et al., 2017
- “Moving Medical Education and Sexuality Education Forward” Carey Roth Bayer & David Satcher, 2015
- The State of Sexual Health Education in U.S.Medicine” S. Criniti et al., 2014.





























Comments are closed.